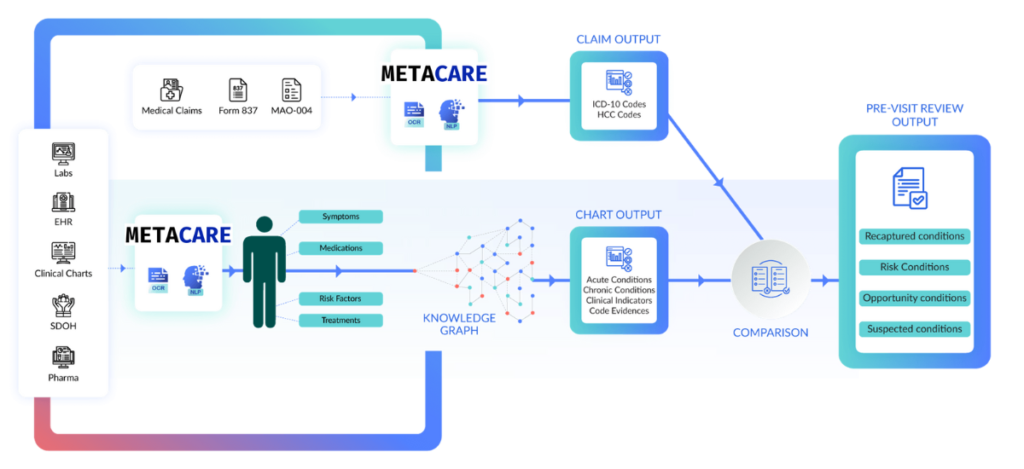
Retrospective chart review solutions provide a comprehensive assessment of patient health histories, leading to more precise risk adjustment factor (RAF) scores.
By analyzing past medical records, these solutions help uncover undocumented or undiagnosed conditions that could impact risk assessments. This ensures that patients receive appropriate care while enabling healthcare organizations to adjust risk scores accurately.
Additionally, retrospective chart reviews identify documentation gaps and missed diagnosis opportunities, helping providers enhance patient outcomes and reduce costs.
Integrating retrospective chart reviews into the risk adjustment process improves RAF score accuracy, enhances care delivery, and optimizes reimbursements for healthcare organizations.