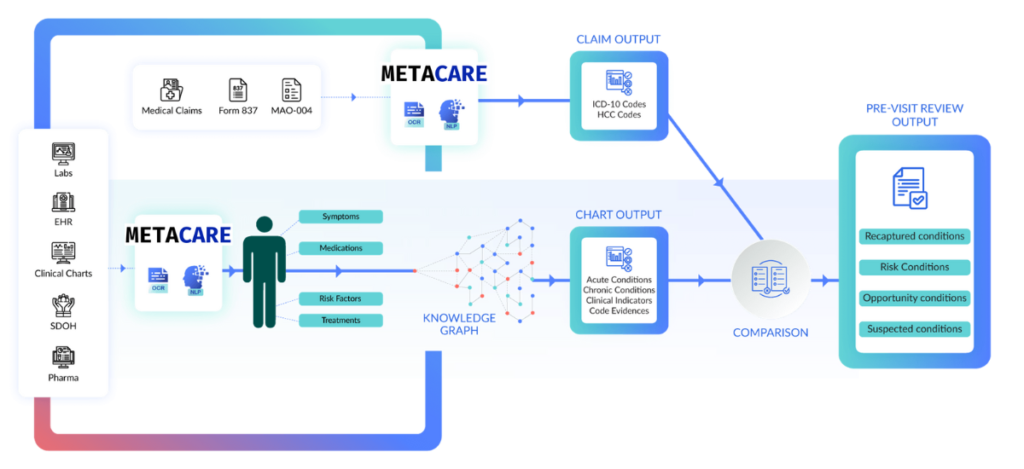
An HCC code audit solution helps detect potential documentation errors or discrepancies that could lead to incorrect RAF scores. Issues such as incomplete records, coding inaccuracies, and insufficient clinical evidence can impact risk adjustment accuracy.
By leveraging an HCC coding compliance solution, healthcare organizations can identify and rectify these errors to maintain an appropriate RAF score. This solution systematically reviews claims data, medical records, and supporting documentation to validate the accuracy of coded diagnoses, ensuring compliance, fair reimbursements, and improved patient outcomes.